提示:文中涉及的治法及用药仅供中医同行参考,患者切勿私自服用,否则后果自负。
导言:有朋友问,学习舌诊在诊断中用处有多大。这是一则旧案,患者临床症状不多,这次主要根据舌象处方用药。但如果能收集更多症状,还是要四诊合参。
一、诊疗背景:当西医束手无策时,中医舌诊如何破解困局?
1. 患者痛点解析
缘起:朋友的弟弟浑身长满了疹子,去西医院诊断为“糠皮孢子性毛囊炎”,开了一大堆西药没治好,情况越来越严重了,求诊于我。如下图:
注:医案保存于大家中医,所以会有大家中医的水印,头面部涉及隐私就不放了
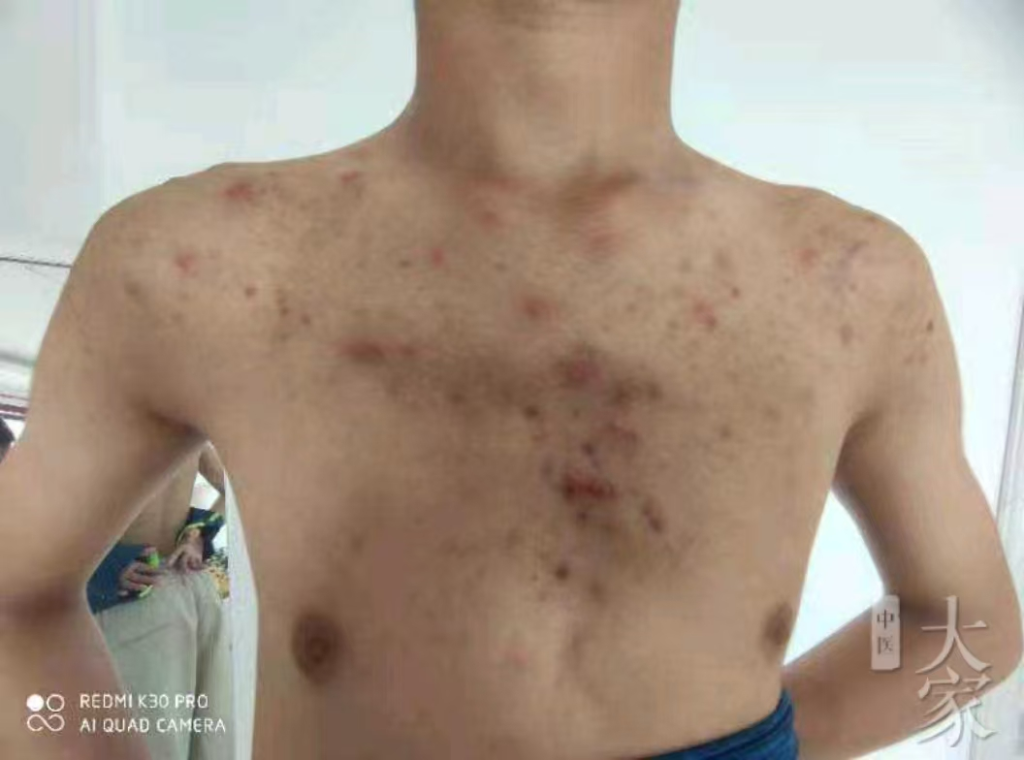
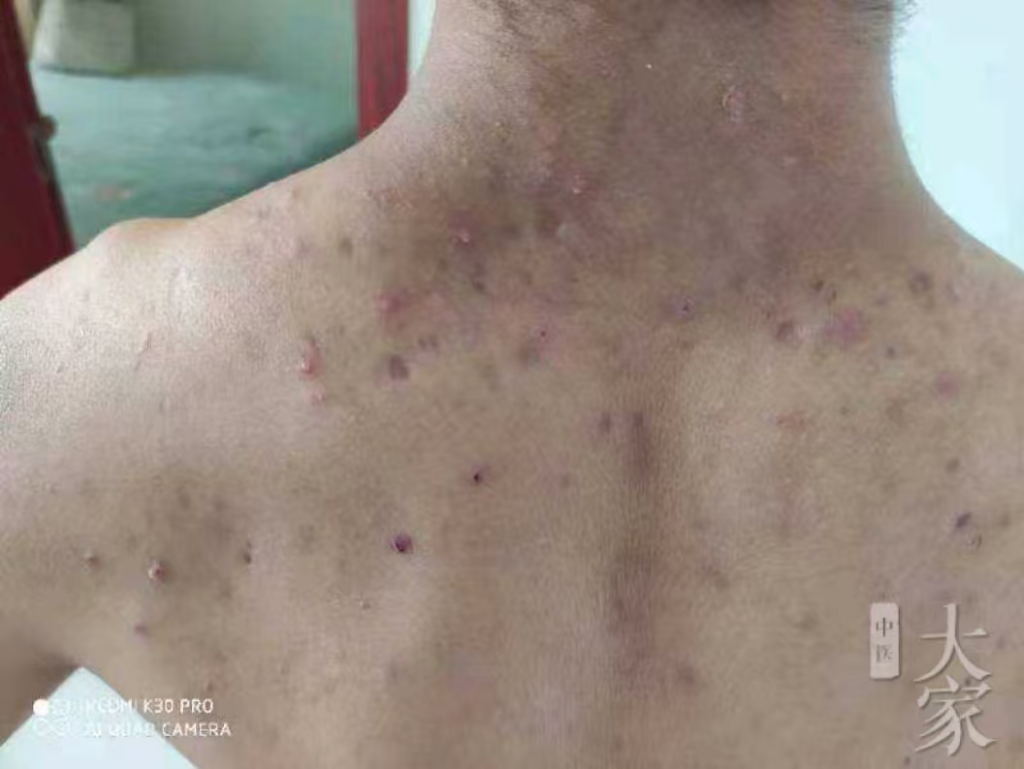
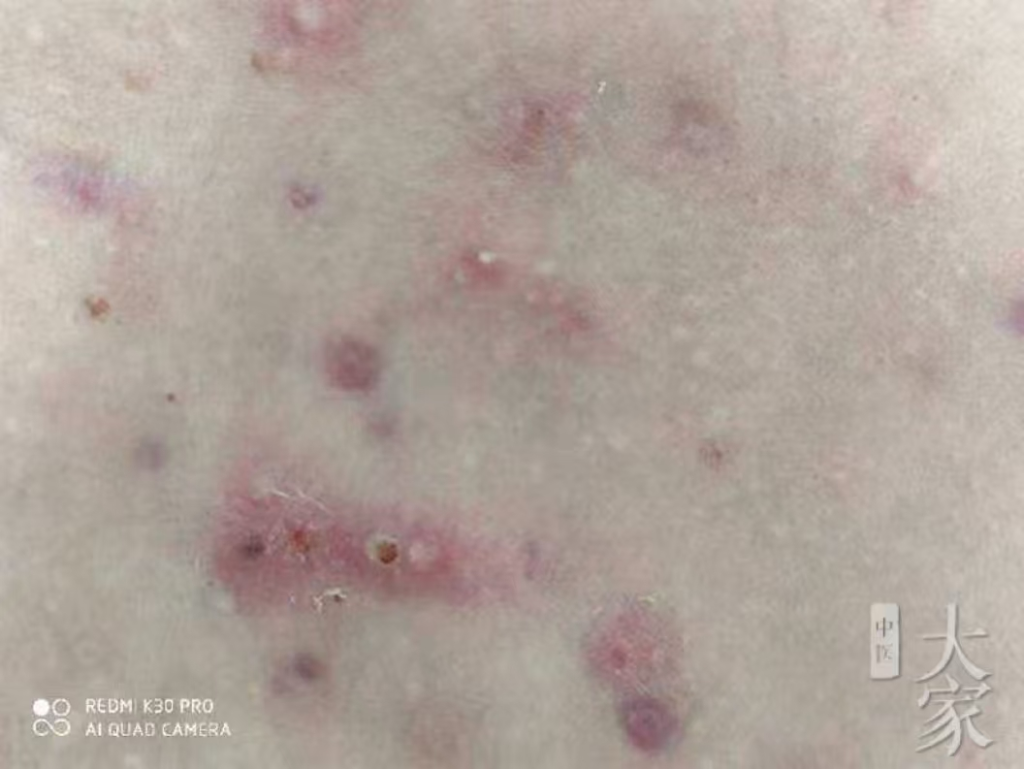
- 西医诊断困境:糠皮孢子性毛囊炎反复发作,抗生素治疗无效。
- 中医辨证优势:通过舌象(轮胎舌+痰浊苔)锁定“肝郁脾虚,痰瘀互结”核心病机。
2. 舌诊核心发现
2024.8.16一诊
现症见:患者男,20岁,前胸,后背、头面部起疹子1年余,纳差、长期便秘,时有胸闷,皮肤瘙痒,时常用手抓,无其它不适症状。由于是网诊,未摸脉。舌象如下:
- 轮胎舌特征:舌周鼓胀如车胎,中间凹陷伴白腻苔(看下图2.16舌诊图)。
- 微观病机:
- 郁结:舌面郁点暗红→气血痰瘀阻滞经络
- 虚证:舌淡嫩边齿痕→脾虚湿盛,清阳不升
二、诊疗全程实录:四诊合参下的精准干预
1. 首诊(2024.8.16)关键决策
2024.8.16一诊
现症见:患者男,20岁,前胸,后背、头面部起疹子1年余,纳差、长期便秘,时有胸闷,皮肤瘙痒,时常用手抓,无其它不适症状。由于是网诊,未摸脉。舌象如下:
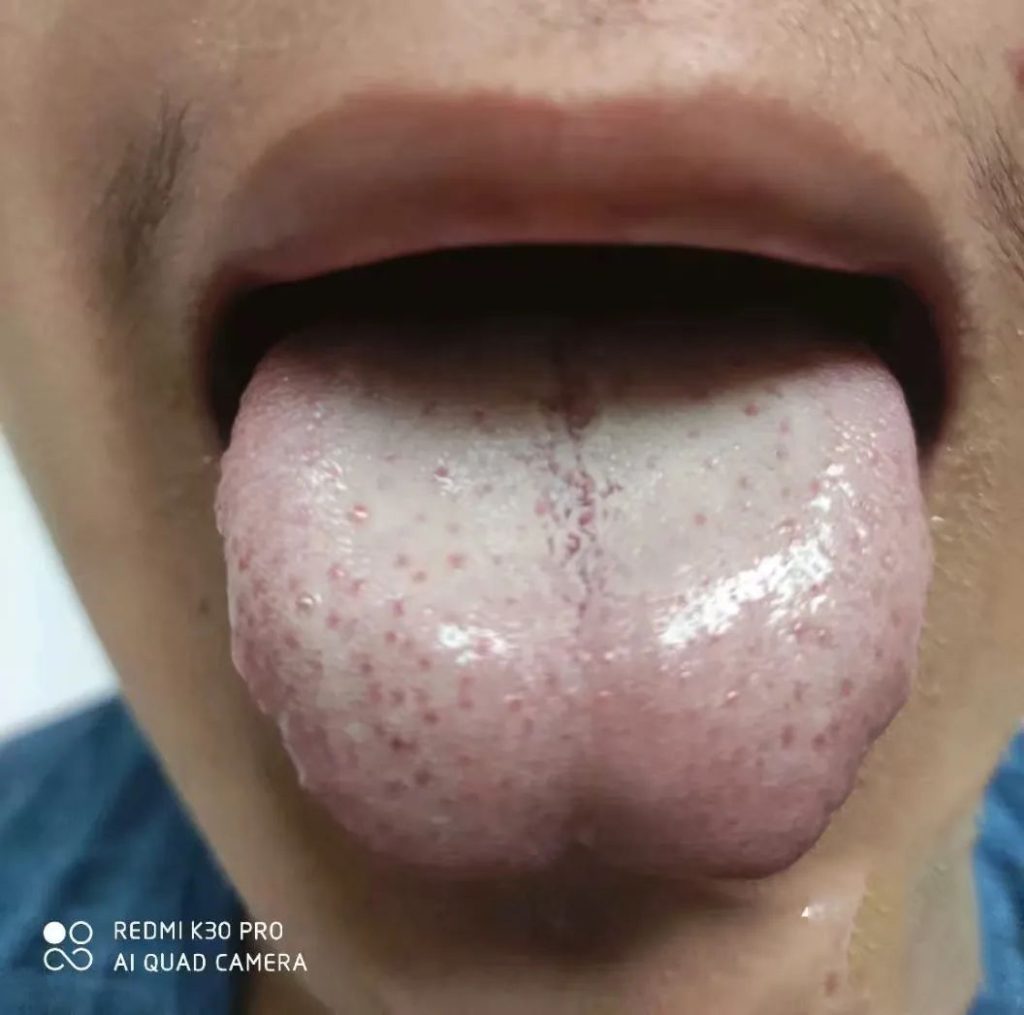
- 舌象分析:这是一个轮胎舌的舌象,舌头周围鼓鼓的,中间凹陷。舌苔白腻,还有痰浊。病机为肝郁脾虚,痰湿内盛。另外舌头上面的郁点很明显,这个郁点不是很鲜红,有点发暗,体内瘀滞也是很明显。
- 症状聚焦:纳差便秘、胸闷瘙痒、疹色暗红。
- 治疗及处方:疏肝健脾,化痰湿,开破郁结。
- 诊方:柴胡20,枳实20,炒山药20,干姜10,白蔻仁10(后下),砂仁10(后下),炒白术15,党参9,茯苓15,皂角1g(打粉),大枣8枚,黑丑6,赤芍10,丹皮10,三棱9,莪术9,焦山楂30,生麦芽20,香附15,陈皮15,川椒4,金银花30,连翘30,元胡10,土茯苓30。
单位:克;共7付,每日一付,分早晚两次温服。
忌油腻,辛辣,寒凉食物。 - 方剂解析:
- 四逆散+四君子汤+行气活血药,另外三路分消,使毒素从表、大便、小便排出。柴胡疏肝解郁,白术健脾燥湿,党参益气升阳。
- 三路透毒法:排毒路径用药配伍作用靶点:金银花、连翘用来透表,使毒素从表走。川椒用来辛散加强透表力量。
三棱、莪术、元胡等活血药开破郁结,疏通走表的道路。
黑丑使部分毒素从大便走。茯苓及土茯苓使部分毒素从小便走。
皂角粉配大枣这是皂角丸,有很强的透破及化痰能力。
土茯苓是皮肤病常用药,尤其适合那种皮肤表面有水泡的病,没有水泡的话也加上,它本身就有解毒的作用,西医称之为抗菌。
2. 复诊(2024.8.23)调整策略
2024.8.23二诊反馈图片如下:
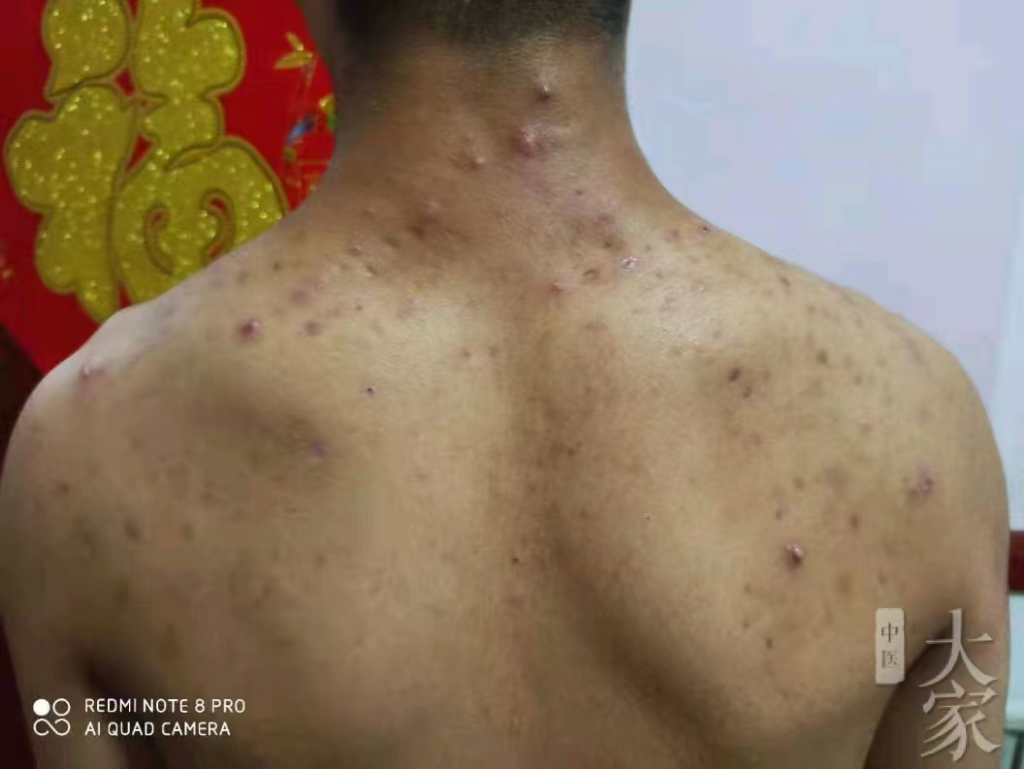
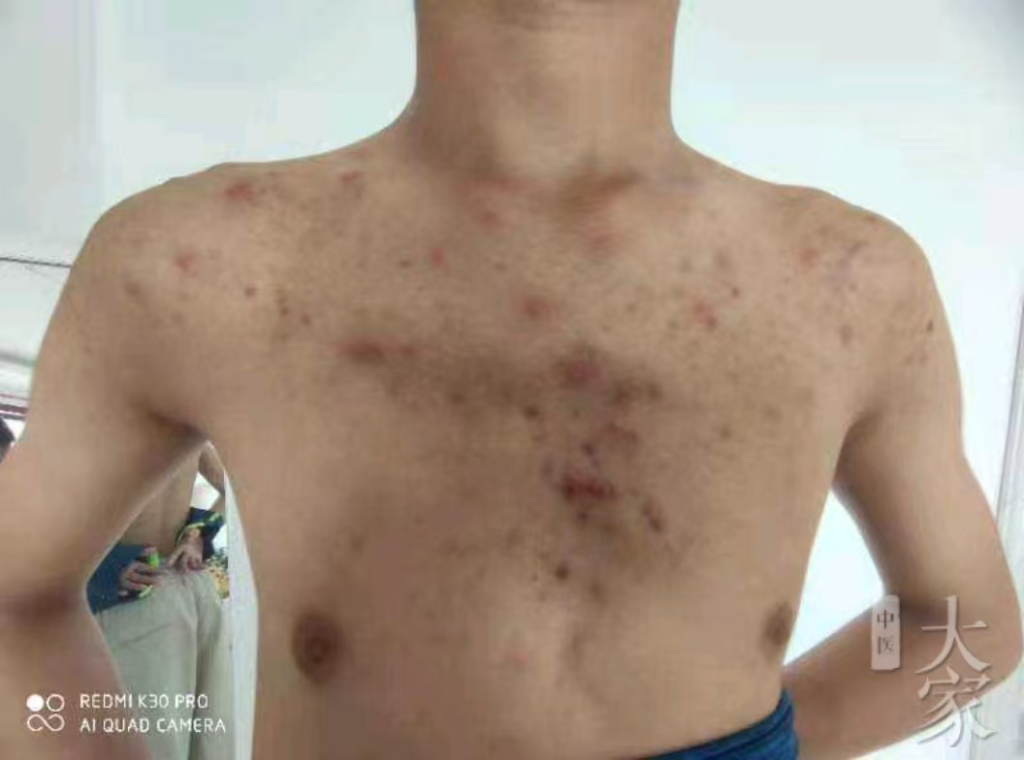
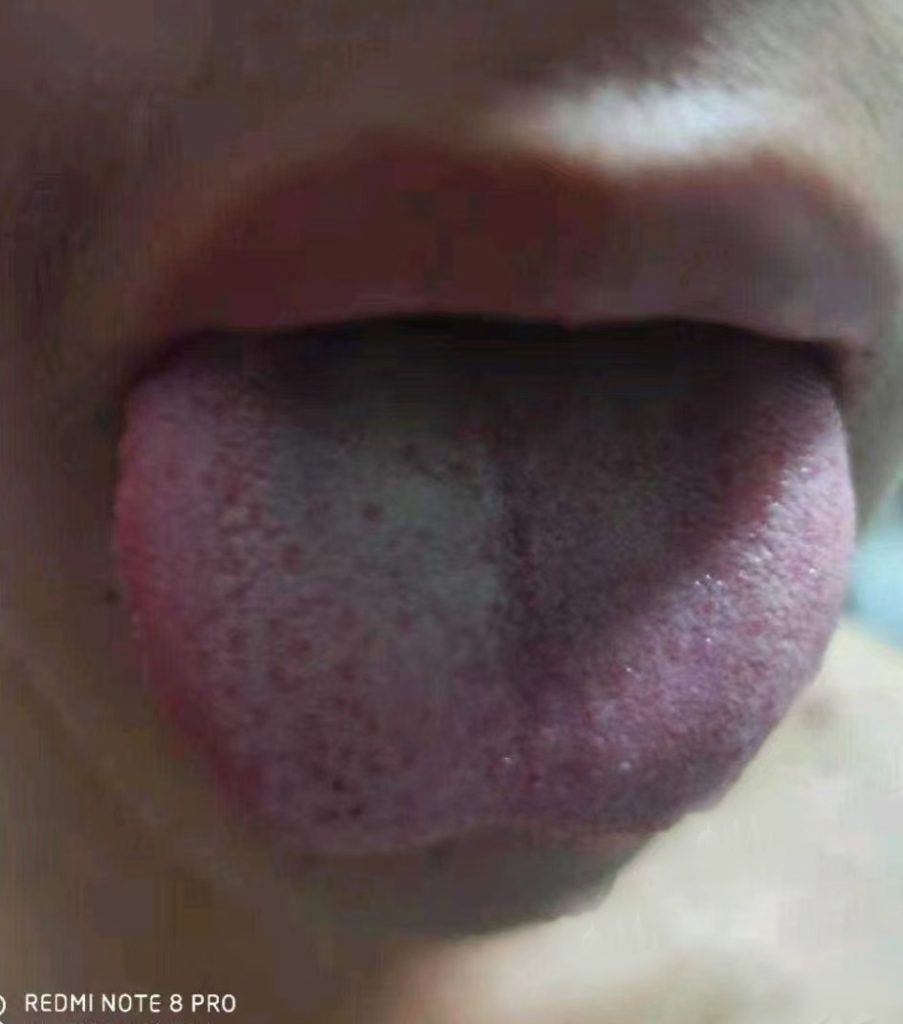
- 从照片上来看,疹子没那么红了,和之前相比变化不是特别明显。但舌象变化很大,痰浊明显少了很多。患者言没那么痒了,大便正常,胃口还行。嘱继续守方7付。
- 舌象改善:白腻苔减少50%,郁点变浅(附舌象图2)。
- 守方优化:加三棱、莪术加强破瘀,焦山楂消食导滞。
3. 疗效追踪(2024.8.31)
2024.8.31服完14天药后反馈如下图:
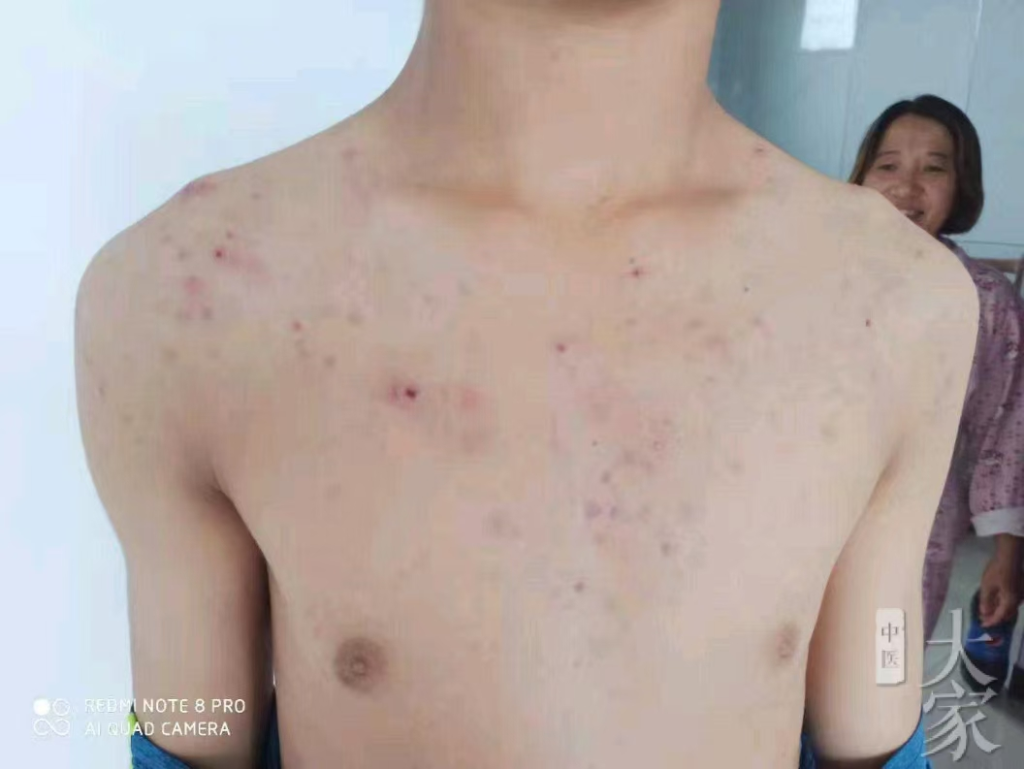
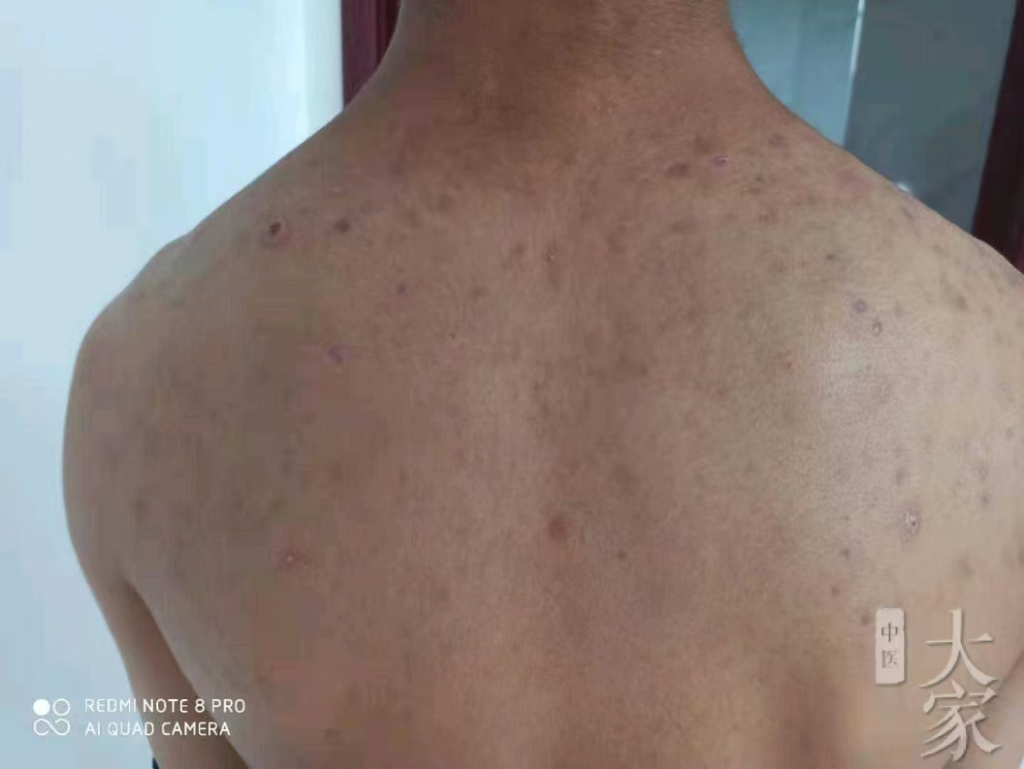
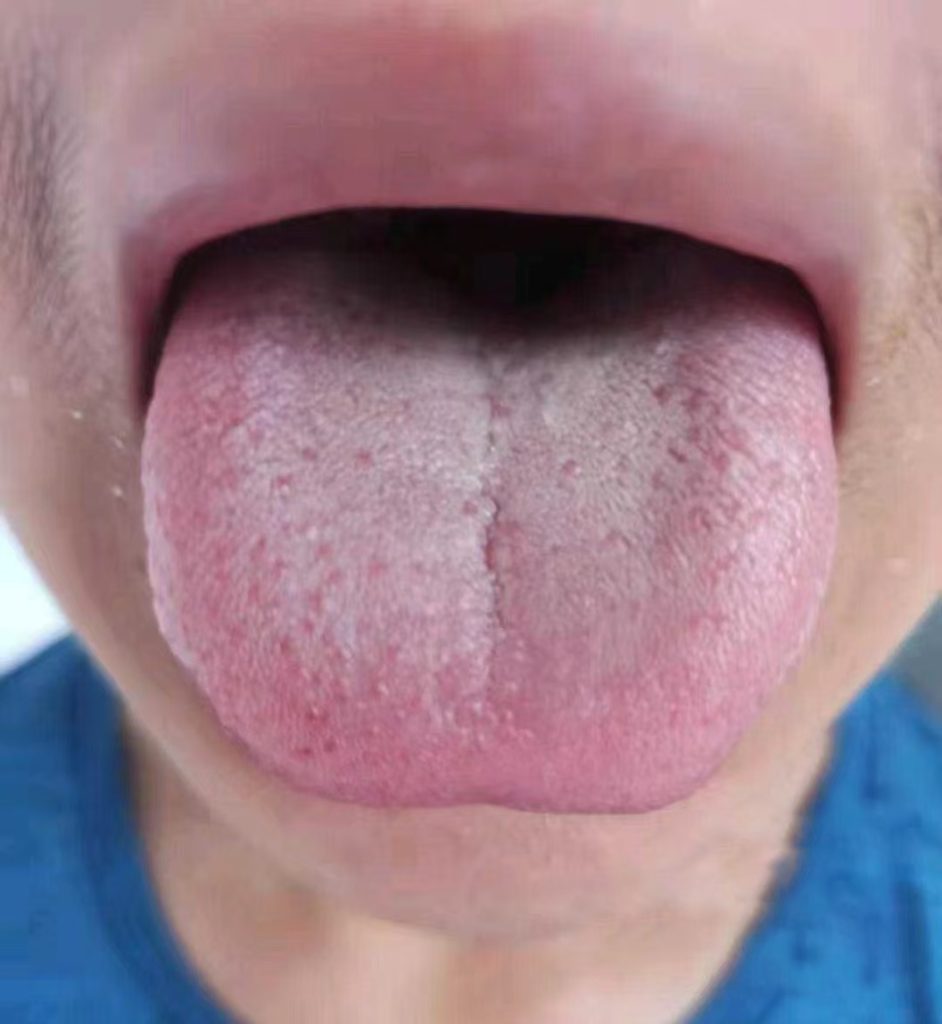
从患者反馈的图片来看,患者身上的疹子基本消除了,不敢说皮肤完全光亮如新,跟患病之前相比变化很明显。
尤其这个舌象上,基本也恢复正常了,遗留点小尾巴问题不大。
患者由于要上学,煎药没那么方便,且他感觉自己问题不大了,不再服药。遵他的意愿,让其服用血府逐瘀丸和逍遥丸一周善后。
3. 回访(2024.9.6)
患者告诉我,他目前皮肤痘痘都消了,也不痒了,胃口很好,大便也通畅,就是自己抓了一年了留下不少淡褐色疤痕。
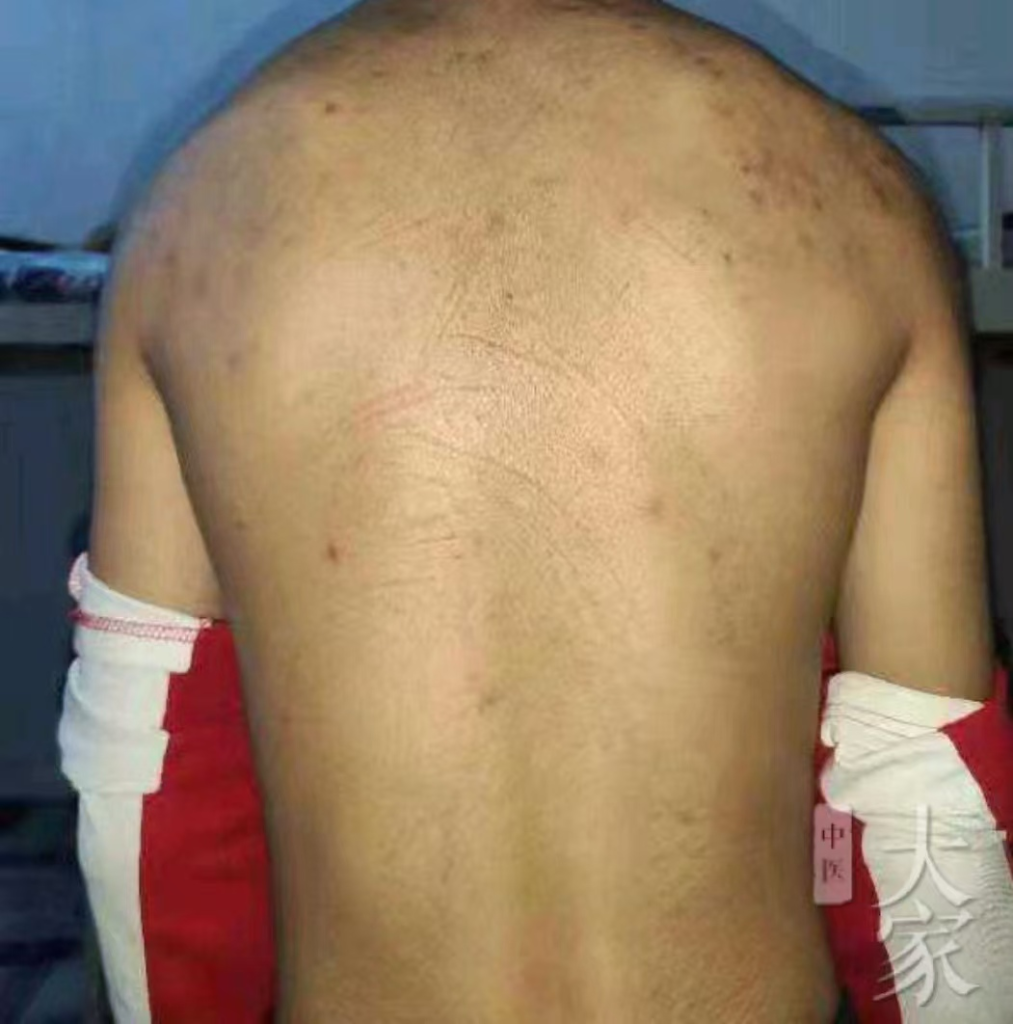
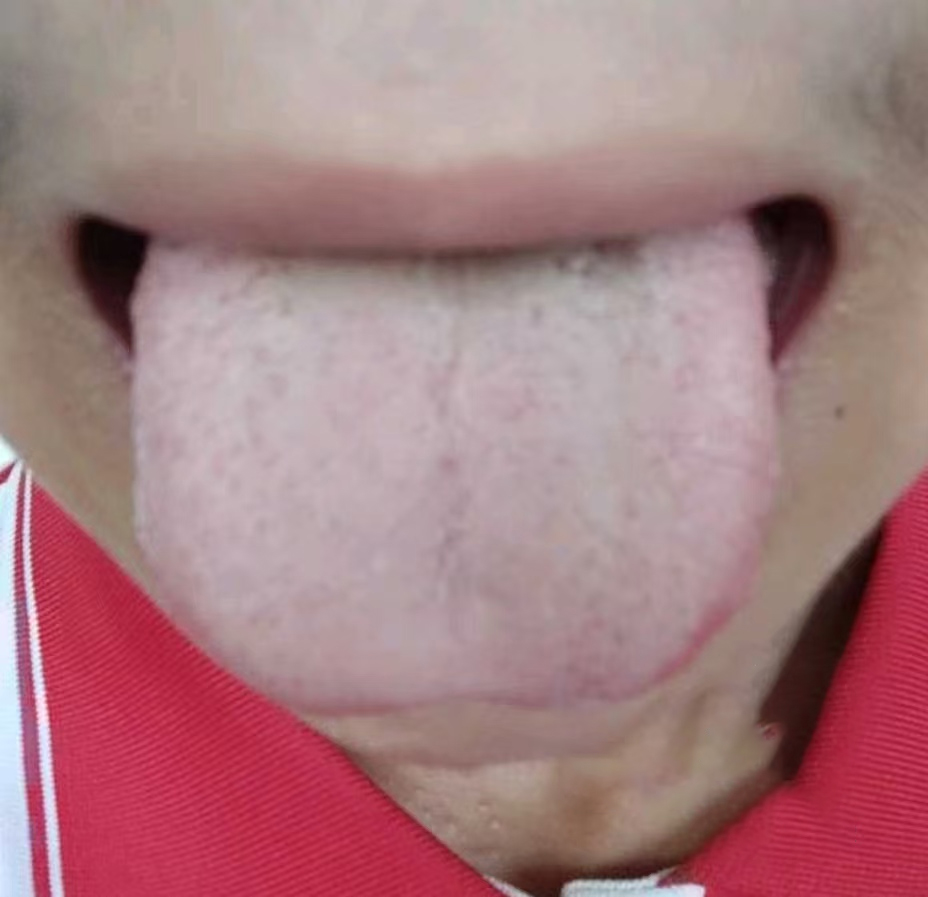
- 皮肤改善:疹退痒止,遗留淡褐瘢痕。
- 舌象复盘:从他反馈的舌象上来看,目前那种壅滞之象没有了,但是有点偏淡白,偏寒,我问他是不是最近老喝冷饮,吃雪糕,他说太热了,不喝不行啊。年轻人啊,还是年轻!
- 只能嘱咐他渴了喝温水,不知道他做到没。
三、经典方剂拆解:从四逆散到皂角丸的配伍玄机
1. 核心方剂解析
- 四逆散(柴胡+枳实+白芍+甘草):
- 现代研究:柴胡皂苷d调节Th17/Treg平衡,抑制毛囊角化(《J Ethnopharmacol》2022)。
- 皂角丸(皂角粉+大枣):
- 透毒机制:皂苷成分促进角质层松解,大枣缓和刺激性。
2. 用药禁忌警示
- 慎用人群:阴虚火旺者禁用温燥药(如干姜)
- 替代方案:痤疮丙酸杆菌感染加蒲公英30g+紫花地丁15g
四、医案启示录:中医皮肤科的破局之道
1. 三大突破性认知
- 皮损本质:痰瘀互结→非单纯“湿热”论治
- 舌诊价值:轮胎舌→肝郁脾虚体质的早期预警信号
- 分消策略:透表+通腑+活血→立体排毒体系
2. 后续调理建议
- 食疗方案:四神汤(茯苓+莲子+芡实+山药)健运脾土
- 外治法:颠倒散(大黄+硫磺)外敷瘢痕部位


发表回复